Irritable Bowel Syndrome (IBS) consists of a number of symptoms. The most common symptoms of IBS are abdominal pain and abnormal bowel habits. Many patients with IBS get crampy abdominal discomfort or pain, which comes and goes, and fluctuates with bowel function (typically easing after the bowel action).
IBS is just about the most common disorder of the digestive system and up to one-third of the population experience symptoms from time to time. It is one of the most common reasons for a visit to the GP. Women are slightly more affected than men and the usual age for patients to seek advice is between 20 and 40 years. As many as one in eight people have symptoms of IBS at any one time.
How does irritable bowel syndrome (IBS) occur?
During digestion, the intestine squeezes its contents along our insides towards the anus. This process (peristalsis) is usually painless and we do not realise that it is happening unless there is an abnormal squeeze within the bowel or, for some reason, the intestine becomes more sensitive. These changes can be quite painful. In addition, patients with IBS seem to have greater sensitivity to the way that their intestines are moving, meaning they feel pain more easily.
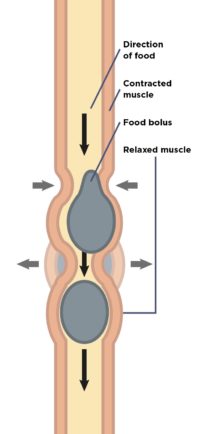
How food (food bolus) moves along the gut.
Causes of irritable bowel syndrome (IBS)
We do not think that IBS has a single cause and there is a wide variety of reasons why patients develop the condition. There does not seem to be a genetic cause, and the single most common trigger to the start of symptoms is following a bout of food poisoning or gastroenteritis. Although the cause is not clear, there are many factors that can provoke symptoms. Some people find that stress makes their symptoms worse. In some people, eating irregularly or eating an abnormal diet may be responsible. Some drugs, particularly when taken long term for chronic conditions, can cause IBS type symptoms such as diarrhoea. Overall, there seems to be some interaction between the nervous system in the gut and brain, emotional state and the immune system of the gut.
What are the usual symptoms of irritable bowel syndrome (IBS)?
Approximately one third of IBS patients suffer from bouts of constipation, one third suffer from bouts of diarrhoea and most other patients don’t fall into a single pattern. The form of IBS that seems to follow gastroenteritis often leads to the diarrhoea type. Identifying these different types of IBS is important because treatments often work quite differently depending upon whether diarrhoea or constipation is the main problem. However, we do know that the pattern of bowel movements can alter over time and this means that your treatment might need to change should your symptoms vary.
Alarm symptoms
These symptoms are not usually associated with IBS but may be associated with other diseases. If you experience any of these you should see your doctor as soon as possible:
- A persistent change of bowel habit for 4 weeks or longer, especially if you are over the age of 40
- Passing blood from the back passage
- Unintentional weight loss of more than 2kg (4 pounds) over a short period of time.
- Diarrhoea waking you from sleep
- Fever
The need to see a doctor is especially important if there is a family history of bowel disease (such as cancer, colitis or Crohn’s disease).
How is irritable bowel syndrome (IBS) diagnosed?
The GP will want to rule out other diseases but will probably be able to make a diagnosis based on the described symptoms. Sometimes IBS symptoms can be caused by drugs you are taking for other conditions. It may be worth discussing this with your doctor to see if a drug switch can be made. Further tests may include blood tests, which will be used to assess
the following:
- Whether anaemia is present
- That the thyroid gland is working properly
- Liver and kidney function
- Any signs of inflammation in the bowel
- Whether coeliac disease may be the issue
Faecal Calprotectin: this is a stool test increasingly used both to look for infection and to help exclude other bowel diseases.
What treatment is available for irritable bowel syndrome (IBS)?
Dietary Management
if a dietary cause is suspected the GP can give advice on what to eat or may refer you to a dietitian. The dietitian will try to identify any foods that cause your IBS symptoms (trigger food). This may involve leaving out particular sorts of foods from the diet, to see whether these symptoms improve. The dietitian may suggest an ‘exclusion diet’, which will exclude a number of common ‘trigger’ foods from your diet. A particular form of this is the low FODMAP diet. If symptoms improve, individual items can then be added back into the diet until the specific trigger food or foods are identified.
If constipation is a symptom, then bulking agents such as natural bran, bran-containing cereals and ispaghula husk (a natural laxative) are helpful. But some laxatives (like fibre or senna), whilst helping with constipation, may make pain a little worse.
Drug therapy
Drugs to reduce bowel spasm have been used for many years. They are generally very safe and often worth trying. Most are available without a prescription and the pharmacist can advise. Unfortunately, they only benefit a relatively small number of patients.
Laxatives can be prescribed for constipation by your GP or from the pharmacist whilst some patients benefit from treatment with peppermint oil or other over-the-counter medicines.
Some patients find probiotics very helpful, but there is no specific prescribed preparation. It is rather a question of trial and error.
Sometimes when pain is a major problem, small doses of drugs, which are used as antidepressants, such as amitriptyline, can be helpful. These can be useful in patients who have no signs of depression. There are also new classes of drugs that may be used if simpler treatments do not succeed.
New drugs are being developed, some of which may help patients whose main symptom is diarrhoea and others who tend to be constipated. Some of these newer agents are not yet available to doctors to prescribe but it does seem likely that a wider range of treatments will be available to patients with IBS in the near future.
What other treatments are available?
- Hypnotherapy and relaxation therapy: these have both been shown to be effective for some people but it is unclear whether they improve bowel symptoms. Hypnotherapy can be obtained through approved therapists who should be members of the British Medical Hypnotherapy Association. Your GP can advise on counselling, and some specialists believe that a psychological treatment called Cognitive Behavioural Therapy (CBT) can be useful.
- Alternative therapies: there are many alternative therapies in the field of IBS, although none of them have any clinical evidence to prove that they do work. Some patients certainly find that herbal remedies can be helpful but at present there isn’t enough evidence to be sure about this. Many doctors are wary of recommending what they see as unorthodox or unproven treatments although few will object if you wish to try alternative medicines.
How can I self-manage my irritable bowel syndrome (IBS)?
Irritable Bowel Syndrome (IBS) is a condition where good self-management can make a huge difference to the symptoms experienced:
- Identifying trigger foods: this may be done by a dietitian. Keeping a food diary together with a record of bowel symptoms may show which foods cause the most problems or whether there is some other pattern. Foods which commonly cause abdominal upset include wheat products, dairy products, onions, nuts and caffeine-containing drinks such as coffee, tea and cola. Some patients cannot digest lactose (the sugar in milk) and so develop wind and diarrhoea after taking large amounts of milk or dairy products, which can include cream, cheese, yoghurt and chocolate.
- Healthy eating habits: avoiding trigger foods and eating regularly and healthily can bring about a significant improvement in symptoms
- Patient support: The IBS Network provides a unique self-care programme to support people living with irritable bowel syndrome. The programme, which is available to members, can be accessed at www.theibsnetwork.org to work through at home, or in IBS Support groups. Members receive access to a telephone helpline, serviced by specialist IBS trained nurses, an email professional response service, recipe ideas, a quarterly magazine and a ‘Can’t Wait’ card to help when out and about. To become a member go to the website or call their office on 0114 272 3253. Their quarterly magazine provides news and information including research updates. There is also a monthly newsletter that contains recipes.
What to ask your doctor?
These are some useful questions you can ask your doctor:
- Have I been fully checked for other bowels conditions?
- Are there any medications that would be appropriate
for me to take? - May I be referred to a dietician?
- Are there any IBS patient groups in my area?
- Can I have a review regularly for my IBS? (See below)
The National Institute of Health and Clinical Excellence (NICE) provide guidelines that doctors can follow when diagnosing and treating people with IBS.
NICE also produce Quality Standards for IBS and these standards show what good service provision should look like. There are four standards currently:
- Considering that people should have had a diagnosis of Inflammatory Bowel Disease ruled out before providing a diagnosis of IBS
- Giving a positive diagnosis depending on symptoms meeting the diagnosis criteria for IBS and not just based on a process of excluding other diagnosis. Testing that may be required is listed.
- Adults getting a referral to a trained practitioner if symptoms continue after first line dietary advice (see the standard) has not been effective to manage symptoms and a restricted or exclusion diet is required. Please note the ONLY trained practitioners are Dietitians registered with the HCPC. This standard can facilitate a referral to a dietitian for a low FODMAP diet.
- Many people live with IBS longer term without knowing about new treatments. This standard is an opportunity for a person with IBS to discuss their symptoms and how these are managed with their healthcare professional. This appointment can take place at a frequency agreed by the person and their healthcare professional, and can take the form that they feel is the most appropriate (such as attending the GP practice or a telephone conversation). Please note you have to request this from your doctor (usually your GP) it is not automatically provided.
This information was originally published HERE and for more support on this condition please visit Guts UK
Where to next? Find out more about Working with clients who have Ehlers-Danlos syndromes.







